Lymphedema 101
Published on April 30, 2021
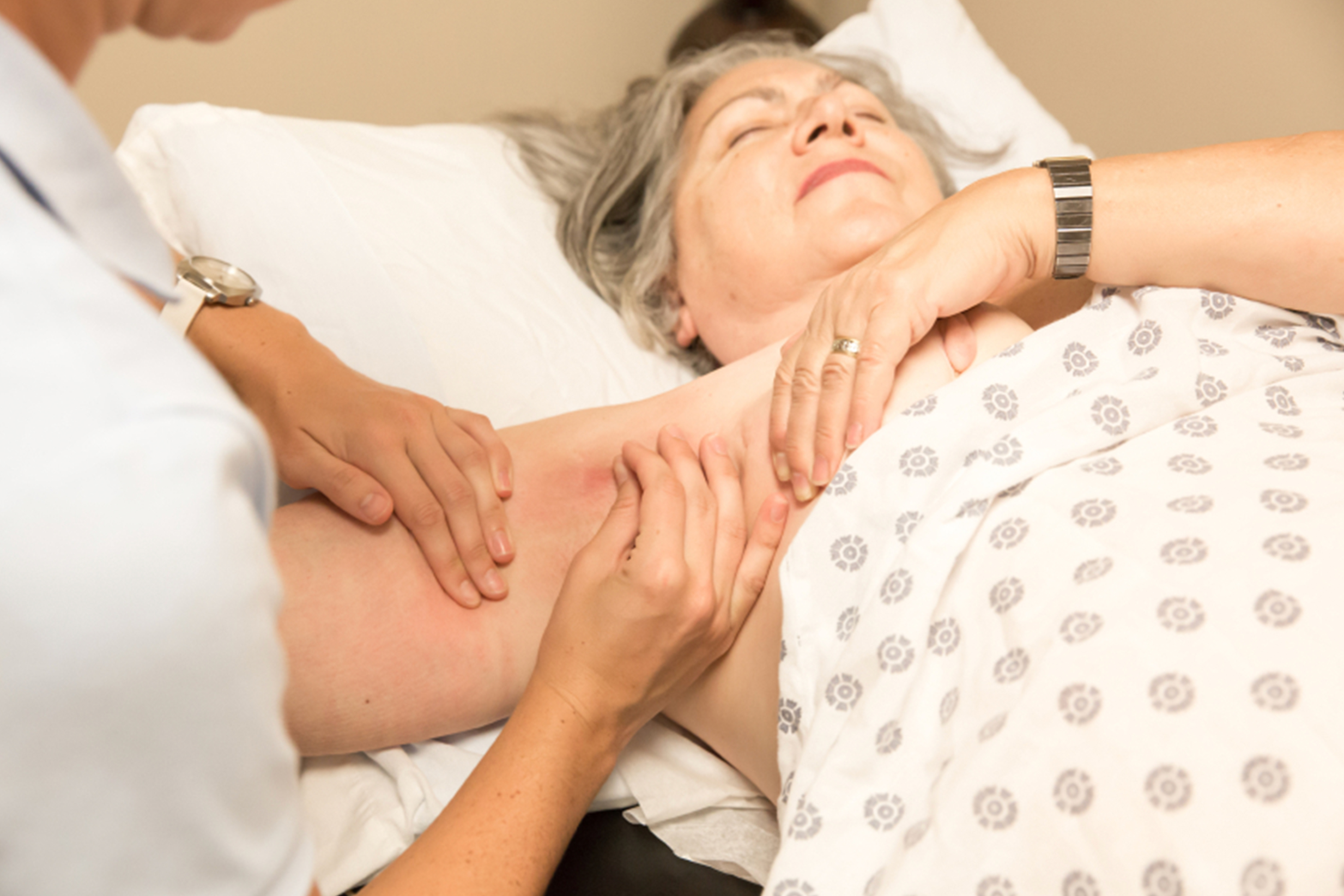
Listen to the episode to hear Marcia explain all aspects of lymphedema, including:
- Sponsor Message
what lymphedema is and where it can develop
- Sponsor Message
risk factors for lymphedema
- Sponsor Message
how lymphedema is treated
- Sponsor Message
steps people can take to reduce their risk of lymphedema or lymphedema flare-ups


Marcia Beck is a clinical nurse specialist at the University of Kansas Health System. Marcia is certified in adult health and breast health and also certified as a lymphedema therapist by the Lymphology Association of North America.
Jamie DePolo: Hello, thanks for listening. Our guest today is Marcia Beck, a clinical nurse specialist for lymphedema at the University of Kansas Health Systems. She is also certified in adult health and breast health and also certified as a lymphedema therapist by the Lymphology Association of North America.
Marcia joins us today to talk about lymphedema: what it is, who gets it, how it’s diagnosed, and how it’s treated, as well as tips to keep lymphedema risk as low as possible. Marcia, thank you so much for joining us to talk about this important topic.
Marcia Beck: Thank you for having me.
Jamie DePolo: So, to start, could you tell us what lymphedema is and where it can develop?
Marcia Beck: Yes. Lymphedema is a protein-rich swelling. Lymphatic fluid is throughout our body, and it can develop when there is a disruption in the lymphatic vessels and it pools, which causes swelling.
Jamie DePolo: Okay, thank you. Now, when we think of lymphedema with our audience, we are talking to people who have been diagnosed with breast cancer, treated for breast cancer, worried about breast cancer. My understanding is that, often, that can happen after breast cancer surgery, but I think also radiation can contribute to lymphedema. So, could you talk a little bit about how it happens in the course of breast cancer treatment?
Marcia Beck: Certainly. We are at risk for lymphedema after lymph nodes have been removed from breast cancer for surgery. So, when we think of a few lymph nodes, such as in sentinel lymph node surgery, is associated with a lower risk for developing lymphedema.
Now, most of those patients do require radiation treatment, which sometimes can increase scarring, which increases the risk for lymphedema.
The greatest risk for developing lymphedema would be for those patients that have had to have many lymph nodes removed, such as an axillary lymph node dissection. The lymphatic fluid can’t really find its true route and may pool more readily after that type of surgery.
Jamie DePolo: Now, before a person has breast cancer surgery, are there characteristics that would put one person at higher risk of lymphedema than another?
Marcia Beck: I think it would be hard to determine individual risk before cancer. You know, we’re all kind of uniquely created with varying amounts of lymph nodes throughout our body. We have 500 to 700 lymph nodes, and each one uniquely created. So some women might have as few as 12 or 15 lymph nodes under their arms. Other people might have 35 or 40, and there’s not really a good method to detect that prior to surgery.
There are some family tendencies for primary lymphedema, and they either are born with fewer lymph collectors or the valves just don’t work as well. And you can see the trends of swelling within family members.
Jamie DePolo: Okay. Thank you. If someone’s been diagnosed and is planning to have breast cancer surgery, are there risk factors, I guess right before the surgery, that may increase the risk of lymphedema? That’s what I was wondering. Like, are there things that somebody could do ahead of breast cancer surgery that may reduce the risk for developing lymphedema?
Marcia Beck: There has been research that showed that a higher body mass index, people that are overweight — greater than about 25 or 30 BMI — are at increased risk for developing lymphedema.
Jamie DePolo: Now, I have read that experts estimate about 20% to 30% of people develop lymphedema after breast cancer surgery and/or radiation. But then again, I’ve also seen estimates that lymphedema numbers range from 10% to 90% of people that have breast cancer surgery. So, in your experience, what numbers are you most comfortable with?
Marcia Beck: Well, I work in an institution that uses prospective surveillance, early detection, and that’s really important in the breast cancer world. So, we estimate that patients that are receiving sentinel lymph node biopsies, nationwide, have about a 6% to 10% chance of developing lymphedema. It is higher for patients that are having an axillary lymph node dissection, so that might be closer to that 40% that you have read.
Jamie DePolo: Okay. Now, lymphedema. I’ve seen on our discussion boards, and people are talking about it and also talking to friends who’ve been diagnosed. Some people have it in their hand and arm, some people have it in their trunk. After breast cancer surgery or radiation, where are the most common places for lymphedema to develop?
Marcia Beck: Well, you know, the lymphatic system divides itself into natural body quadrants, so the area that the quadrant drains. So, on the upper body, it’s divided right down the breastbone to the belly button, and it follows the rib cage around to the spine. So, whichever extremity has had the lymph node dissection, that whole quadrant could potentially have swelling, or lymphedema, because it's all trying to drain to the lymph nodes under the affected arm.
Most commonly, it usually starts in the extremity. You know, gravity works, so swelling may pool, and maybe the first sign might be some fullness in the hand. Very early signs that we try to educate our patients about might be just an unrelenting aching between the shoulder and the elbow on the affected side, prior to there ever being any signs of swelling. So, we want people to be aware and listen to their body.
Jamie DePolo: Okay. Okay. That’s good to know. Now, I’ve also read that some therapists that specialize in lymphedema recommend that any woman who’s having breast cancer surgery have her arm, or both arms if she’s having a double mastectomy, measured before surgery — in other words, the circumference of the arm and the hand — so that there are baseline measurements, and then any swelling can be tracked. Do you find this helpful?
Marcia Beck: I do. I do feel that a preliminary measurement — circumferential measurements can be a little subjective. There are now some tools that are being utilized to measure lymphatic flow, like the ImpediMed bioimpedance spectrometer is an excellent tool to help measure, and a baseline is really essential.
And when we do circumferential measurements, we do both arms. You know, your arms are not necessarily the same size. Sometimes the dominant arm is a little larger than your non-dominant. So having those baseline measurements prior to surgery is very helpful.
Jamie DePolo: Okay. I do have a question. The tool you mentioned — and I’m going to get the name wrong — but the flow cytometer, if that’s right. Could you tell us a little bit about how that works?
Marcia Beck: The bioimpedance spectrometer is actually a scale. The brand name for that scale is SOZO, it’s put out by the ImpediMed company. It actually sends a little tiny electrical current that kind of maps lymphatic flow, and it can measure increases in fluid. So, after patients have recovered from their surgery, we can put the patients back on that scale and compare their measurement to their baseline measurement. And if there’s not a great deal of elevation, we know they’re staying within a normal range, and that’s an excellent medium to help us control or identify early lymphedema.
Jamie DePolo: Oh, that’s interesting. So, if I’m understanding correctly, this machine, it’s actually measuring the flow of the lymph fluid, not necessarily the circumference of the arm. So it sounds like it could diagnose any increase in lymph fluid a lot earlier than a circumference measurement could?
Marcia Beck: Yes. We do try to do both measurements, particularly prior to patients that are going to have neoadjuvant chemotherapy, having some medication prior to surgery. Sometimes those medications can cause swelling as well. So, in addition to measuring with the bioimpedance scale, we also do limb-volume measurements to have both of those on file.
Jamie DePolo: Oh, okay. Very interesting. Thank you. Now, is there an average time after breast cancer surgery when lymphedema develops? I have heard that it can happen years after surgery, but I’m wondering, on average, should somebody be looking, say, a week after, a couple of months after?
Marcia Beck: Yeah, I don’t think immediately after surgery is the main concern. You know, you can have some swelling just in postoperative healing. Research tells us that if lymphedema is going to develop, it’s usually about 7 to 8 months after surgery, so we kind of time our measurements to coincide with that amount.
Now, because lymph nodes do not regenerate, patients are at risk for developing lymphedema, so that’s why the risk reduction strategies and protecting the skin so there’s no infection that could lead to lymphedema.
Jamie DePolo: Okay, and we are going to get to those risk reduction things and the treatment. I am wondering, too, how long can lymphedema last? Is this something that, if it develops, it’s going to be kind of an ongoing thing, or can it be treated and then it goes away. What is your experience?
Marcia Beck: As I mentioned with prospective surveillance and catching things very early, if we catch lymphedema in the very early stages — we call it subclinical, or even stage 1 — it can be reduced or eliminated. Once it’s progressed to stage 2 and has developed some fibrosis, then it’s considered more chronic and not curable. It can certainly be maintained a little bit better, but it is not going to be totally eliminated. And lymphedema can be a progressive disease, so without treatment, it could certainly progress to more difficult stages.
Jamie DePolo: Okay. Thank you. So how is lymphedema treated? I’m assuming that some of the treatments, it’s based on how severe or the stage of the lymphedema, but could you give us sort of a run-through on the basic treatments?
Marcia Beck: Certainly. Now, with prospective surveillance, we are working with the patients to identify early signs, if they’ve had any infections, things like that so that we can treat that immediately and reduce or eliminate that risk.
Once lymphedema has progressed to about a stage 2, they really need to have treatment. The standard of care for lymphedema is called complete decongestive therapy. It’s provided by therapists who have had specialized training in lymphedema: In the anatomy and physically training in lymphedema.
Complete decongestive therapy kind of involves four parts. There’s a real gentle massage-type treatment that’s called manual lymph drainage that trains the lymphatic fluid to use an alternate or adjacent quadrant to drain better.
Then there’s the compression therapy, short, stretch bandages so that the fluid does not re-enter the extremity. Exercise is important while they have the bandages in place.
And then skincare is essential, because breaks in the skin are a portal of entry for bacteria, and that protein-rich lymphedema fluid is just an excellent growing medium for bacteria.
So, it’s kind of four parts provided, and then the therapist, in treating them over a month or 6 weeks, teaches the patient how to care for that in their own home. So a self-care portion of that education as well.
Jamie DePolo: Okay. And then, I guess if someone has lymphedema — and you mentioned it can be chronic, or ongoing — does the person continue to see the lymphedema therapist, or is that something that once the person has learned from the therapist what to do, that the person can do the home care and that can sort of keep it under control?
Marcia Beck: Usually that can keep it under control, and unfortunately, a lot of times it’s our insurance reimbursement or lack thereof that dictates how much therapy can be provided. Some patients really need more assistance than others. Other patients can manage that self-care themselves and should be able to spot check or have a follow-up visit as needed to check on their progress.
Jamie DePolo: I see. Okay. Now, what is the best way to find a certified lymphedema therapist?
Marcia Beck: There are several schools now throughout the United States that offer training for lymphedema therapists. My recommendation would be that it be a certified lymphedema therapist. We have a national certification board through the Lymphology Association of North America. There is a website, CLT-LANA.org that lists therapists that have, voluntarily, sat for a computerized certification test, and I think that’s a very good way to find good therapists that have had the extra training, that have taken the time to sit for a certification to prove that they have entry-level competence to provide lymphedema therapy.
Jamie DePolo: Okay, thank you, because I know in some cases, people get referred to a physical therapist. And I’m not saying that physical therapists are not good, but they may not have that extra training in lymphedema. So, if somebody can’t find, say, a certified lymphedema therapist close enough to them, is it fair to — say if they are referred to a physical therapist — is it fair to ask the physical therapist how much experience with lymphedema the person has?
Marcia Beck: Absolutely. I would highly recommend and question what type of experience does your physical therapist/occupational therapist have in dealing with lymphedema.
Jamie DePolo: Okay. Good to know. Now, I know there’s been a lot of discussion about exercise, and you just mentioned that there are certain exercises that go along with treating lymphedema. But I guess I’m talking about sort of general, other exercise, like specifically weight lifting and lymphedema. And I’m wondering if you could tell us what the current research shows. Because I know, in the past — I haven’t talked to any friends who have been told this lately — but in the past, some of my friends were told, “You cannot pick up anything that’s heavier than a gallon of milk.” But it was because they were told that that would make lymphedema worse or could bring on lymphedema. So, I’m wondering how the research and experience has progressed on that.
Marcia Beck: Yes, we’ve had excellent research in the last several years regarding lymphedema and exercise. Dr. Katie Schmitz has been very prolific in some of her research. There was a PAL trial — it was called Physical Activity and Lymphedema, or PAL, trial — and that has been pretty instrumental in identifying that exercise, in fact, does not increase lymphedema. Now, we need to understand we need to listen to our body, exercise should be supervised, but we want patients to use their extremity. We want them to get back to doing activities they have done previously.
You know, if it’s a weight-lifting situation, we might want to start very slowly. Start with the lowest weights, even though maybe you were working with much higher weights than that. Start with lower weights, maybe fewer repetitions, and see how your extremity feels and work upwards toward your previous normal.
Jamie DePolo: Okay. Good to know. And I’m assuming, too, that if somebody is working with a trainer, they should definitely let that trainer know that they either have lymphedema or are maybe at risk for developing it.
Marcia Beck: Correct. One of the things I might mention here is patients that have had the axillary lymph node dissection, we do recommend they wear a compression sleeve for repetitive activities, and that would include weight lifting. That might include power walking or their elliptical machine, just to provide a little extra support to an extremity that has had additional lymph nodes removed.
Jamie DePolo: Okay, and this is sort of a slight detour, but I know a lot of people are concerned about flying, although right now in this time of COVID, flying isn’t really recommended. But a lot of people who are at risk of lymphedema or have lymphedema are very concerned about flying because of the pressure in the airplane and the change in pressure. What does the research show now? What are your recommendations for that?
Marcia Beck: There is not a lot of research about air travel and compression or air compression changes in the plane. However, we do recommend those patients that have had the axillary lymph node dissection, that they do wear a compression sleeve for air travel. Applying it maybe 30 minutes before you get on the plane, wear it throughout the flight, then as you’re exiting the flight leave it on for another 30 minutes or so prior to taking it off.
We do not recommend patients that have had just sentinel lymph node biopsy surgery, we don’t recommend that they wear a compression garment for either exercise or for air travel. We feel like their lymphatic system will be able to accommodate.
Jamie DePolo: Okay. And I guess I’m wondering, too, if somebody wears a compression garment and maybe it’s not needed, are there any risks with that? Can it be harmful?
Marcia Beck: My concern with people that don’t really need a compression garment is that they might just be purchasing one off the shelf, and it really doesn’t fit properly. So, if it’s too tight, say in the upper arm, or too long and pressing in the wrist, it could actually trigger some swelling in another part of the arm. If you need to have a compression sleeve, it needs to be properly fitted, measured, be sure it’s the right length and size, and the compression strength that’s recommended by your physician or therapist.
Jamie DePolo: Okay. Okay, thank you. That’s very good to know. Now, I did bring up COVID, and I do want to ask, too, because we are living in this time of COVID. Some experts have suggested that women who have lymphedema or are at risk of lymphedema not get a COVID vaccine in the arm on the same side as their surgery and instead ask for the vaccine in the thigh. Is this well known and accepted by vaccination sites? We have heard some of our community members say, “I tried, and the person who was giving the vaccine said, ‘No, I can’t do that.’” What’s been your experience? How are you advising the people you work with?
Marcia Beck: With patients that are at risk for lymphedema, again, if you’ll remember we talked about it, usually just one quadrant of the body. So, the affected arm in that quadrant is what we try to protect, not just from the COVID vaccine, but from other potential needle sticks. So, vena punctures, even those automatic blood pressure cuffs, can sometimes provide too much pressure. But there would be no problem in getting the vaccine in the unaffected arm.
I’ve not really heard of people asking for the vaccination in the thigh, but certainly in the ventral hip area. You know, you can just pull the top of your pants down, and get the ventral hip area there, and that vaccination should be fine. And I can’t imagine anyone saying they could not provide that. In the thigh, I think, would be difficult.
Jamie DePolo: Okay. I see. I see. Yeah, and I guess I was just thinking, too, if somebody had had a double mastectomy and lymph nodes removed on both sides then both arms are out, so where does that leave them. But you’re saying that the top of the hip sounds like a good place.
Marcia Beck: Absolutely.
Jamie DePolo: Okay. Okay. Now, finally, you’ve given us a lot of good information, and I thank you so much. I’m going to kind of ask you to do a little wrap-up. So could you give us some steps that people could take before surgery? They’ve been diagnosed with breast cancer, they know they’re going to have surgery, so are there steps that they can take to reduce their risk of lymphedema at that time? And then also — this is kind of a two-part question so I apologize. If they have been diagnosed with lymphedema, are there steps they can also then take to reduce flare-ups?
Marcia Beck: All right. Well, certainly, when you are initially diagnosed with cancer, communicating well with your physician. Perhaps, having a nutritional consult. As we know, obesity is becoming more rampant in the United States. We don’t recommend a very strict weight-loss program where you’re going to lose 20 pounds in a month, but a well-balanced nutrition program is best. You need good nutrition to heal, so it doesn’t make sense to be very restrictive during treatment.
Certainly, trying to have an optimum body weight reduces the risk for developing lymphedema. If it’s people that have not done much exercise, starting with something like yoga and Pilates that is helping stretch muscles, is focusing on deeper breathing, which is effective for the lymphatic system, could be excellent ways to try to help reduce the risk for lymphedema.
Once you’ve had your surgery, ways to reduce flare-ups is certainly paying attention to your body. If you’re having that unrelenting aching for a couple of days in the back of your arm. If you’ve noticed that you got a bug bite or a sunburn, those sorts of things can certainly be prevented, so any preventive thing you can do. Wearing sunscreen when you’re outside. Wearing bug repellent when you’re out. Being careful when you’re cooking that you don’t stir and splatter hot liquid onto your affected extremity.
Pets in the house — be careful with any scratches on your affected extremity. Clean it really well with soap and water and maybe a little topical antibiotic to keep from having infection. Infection is our main concern that goes onto develop lymphedema.
Jamie DePolo: Okay. Okay. Excellent. Marcia, thank you so much. This has been such great information and really, really helpful.
Marcia Beck: Well, thank you for having me. I certainly appreciate it.
Your donation goes directly to what you read, hear, and see on Breastcancer.org.