Histotripsy for Breast Cancer in the Liver
Published on April 28, 2026
Dr. Brock Hewitt is a surgeon who specializes in treating cancerous and non-cancerous tumors in the liver and other internal organs. One of the techniques he uses is histotripsy. He’s published a number of papers on the procedure and its effectiveness.
Listen to the episode to hear Dr. Hewitt explain:
- Sponsor Message
how histotripsy works and why it’s only used to treat liver tumors
- Sponsor Message
how doctors decide if histotripsy is right for someone with liver metastases
- Sponsor Message
the risks and benefits of histotripsy
- Sponsor Message
insurance coverage for histotripsy
Scroll down to below the “About the guest” information to read a transcript of this podcast.
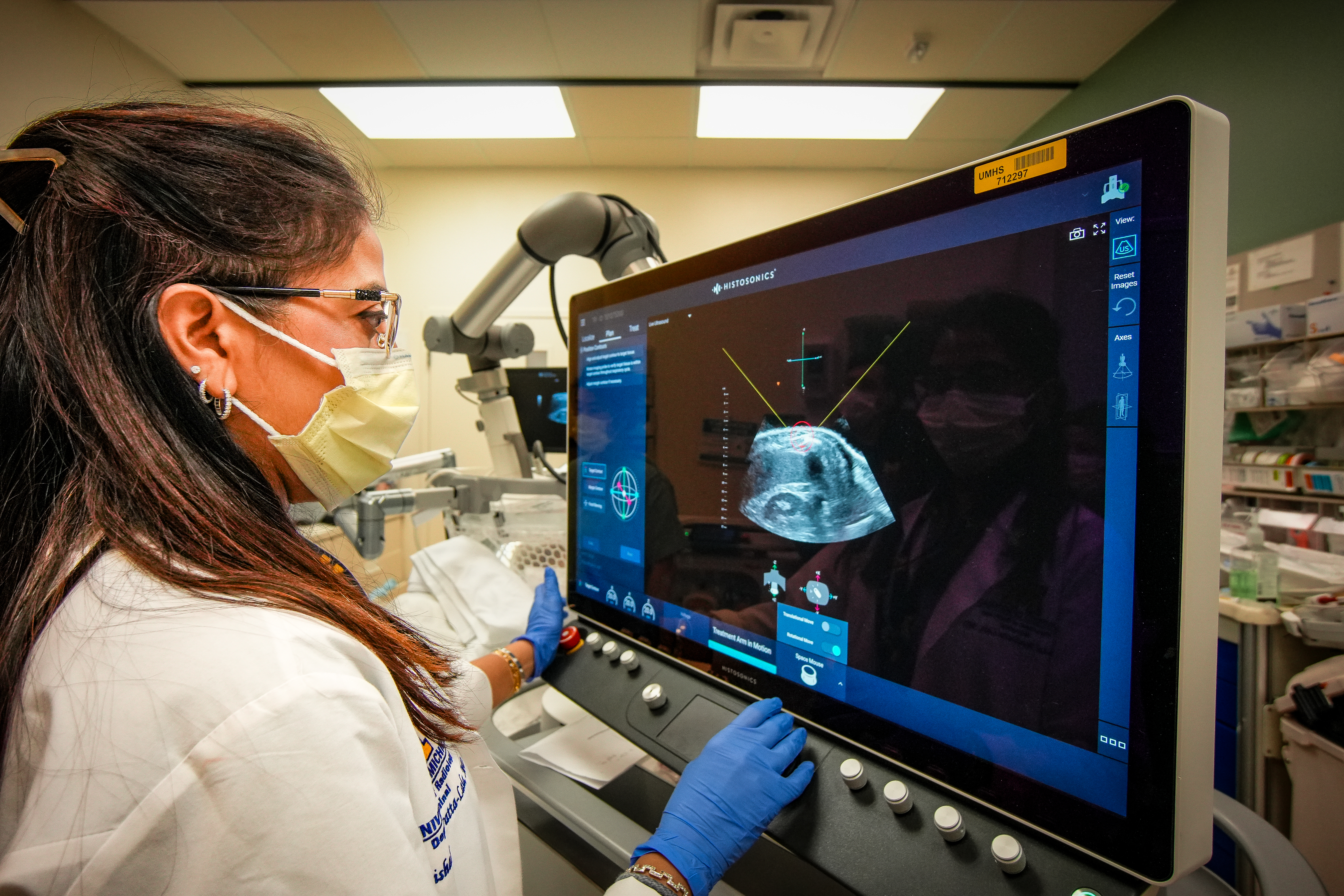
Podcast image credit: Eric Shaw, University of Michigan Office of the Vice President for Research

Brock Hewitt, MD, MPH, is a hepatobiliary and pancreatic surgeon at NYU’s Perlmutter Cancer Center and assistant professor of surgery at the NYU Grossman School of Medicine. He specializes in treating cancerous and non-cancerous tumors in the liver, bile ducts, pancreas, and stomach.
Welcome to The Breastcancer.org Podcast, the podcast that brings you the latest information on breast cancer research, treatments, side effects, and survivorship issues through expert interviews, as well as personal stories from people affected by breast cancer. Here’s your host, Breastcancer.org Senior Editor, Jamie DePolo.
Jamie DePolo: Hello, as always, thanks for listening.
Histotripsy is a procedure that uses ultrasound to treat tumors in the liver. I'm joined by Dr. Brock Hewitt, a surgeon at NYU Langone, who specializes in treating cancerous and noncancerous tumors in the liver, bile ducts, pancreas, and stomach. He joins us today to explain histotripsy and how it’s used to treat breast cancer lesions in the liver. Dr. Hewitt, welcome to the podcast.
Dr. Brock Hewitt: Thank you so much for having me. It’s truly an honor.
Jamie DePolo: So I have to admit, this topic came from a member of our community, and I did not really know much about histotripsy. So I did a little research, and I believe it was approved in 2023. So it’s relatively new. So could you give us a little bit of the history of the procedure? How was it invented? Why is it only used for the liver and not other organs? Just, if you could give us a little bit of background.
Dr. Brock Hewitt: You're correct. So, it was FDA approved in October 2023, but it’s a technology that’s been around for a number of decades now. It was initially kind of started at the University of Michigan and kind of created there in early 2001. And so, it’s been around, like I said, for now for almost over 25 years and it’s kind of gone through a process of extensive testing all the way through, you know, on small animals to larger animals, and over the last couple of years on people.
Jamie DePolo: Okay. And why only the liver? Why not other organs?
Dr. Brock Hewitt: Yeah. Great question. So, the liver…there’s a couple reasons for that. One is related to the mechanism of how it works, which we’ll talk about in a second, and another is practical.
So histotripsy, the design of it right now, is to treat primary and secondary tumors in the liver. So tumors like a liver cancer that started there or tumors like a breast cancer or colon cancer that spread to there. So it happens to be the most common organ in the abdomen where disease spreads to. So it ends up being one of those situations where there’s a lot of opportunities to help patients as opposed, if you chose something, you know, like the kidney, for example, not many lesions will spread there. So, that’s more of a practical reason.
The other reason is that histotripsy right now is designed and the mechanism supports its activity in solid organs. So that would be things like the liver, like a kidney, like a pancreas. The opposite of that would be something called a hollow viscus, which would be something like the stomach or the intestines, like the colon. So those are structures that are hollow on the inside. And air is not histotripsy’s friend, which is interesting because that directly relates to its mechanism of action. So, it’s kind of an ironic point.
Jamie DePolo: So, how does it work? What is the mechanism of action?
Dr. Brock Hewitt: Yeah. So in all of our tissues, even our solid organ tissues, we have these very tiny microbubbles. And the way histotripsy works, as you kind of mentioned, it’s ultrasound-guided ultrasound technology. So what happens is, the device goes over your body. It goes within a water medium, or a water bath, and ultrasound waves are projected through the body, so it is completely transcutaneous, means it goes through the skin. There’s no incisions, anything like that. And it focuses on an area within the organ itself. And at that area you get these pulses of ultrasound. So, on-off, on-off, on-off, many times during one second. And what happens is, those pulses of ultrasound create changes in pressure and it’s those changes in pressure that cause the natural-occurring small air bubbles in our body to expand and contract rapidly. And so, you can think of it like bowling balls bouncing around in a way.
And what happens is, is those air bubbles cause tearing within the cells themselves. And so the cells are essentially torn apart. So it is a mechanical disruption, not a thermal disruption. So that’s what kind of separates it from traditional ablation therapies. Something like radiofrequency ablation, microwave ablation, and histotripsy, they’re all ablation technologies. But microwave and radiofrequency, the intent, or the way in which the tumor is destroyed, or the tissue is destroyed, is with heat. It gets very hot and it burns everything within a certain radius. Whereas the way histotripsy works, is it focuses that ultrasound on an area that causes changes in pressure. That pressure then causes the mechanical disruption of the cells, and the cells are essentially destroyed. And the tumor doesn’t spread because of that. Just because the cells are destroyed.
It’s a common question: Is that if the cells are destroyed does that mean the tumor spreads like a bacteria, like you open it up and it spreads everywhere? It doesn’t happen that way. That cell is dead. That cancer cell is dead so it cannot spread. And then, for example, in the liver, the surrounding tissue that is not destroyed, as it’s quite a precise technology, then goes in and cleans up the mess, so to say. And what we call that is, that’s an acellular lysing. That is what’s left over after the treatment. So, all the cells are lysed, which is another term for broken up.
Jamie DePolo: Okay. Okay. Very interesting. So it doesn’t work in, say, organs that are hollow because there’s too much air. Is that…
Dr. Brock Hewitt: Yes. So, well…kind of. Well, one would be that again, say you have a tumor in the wall of the intestine and that tumor is destroyed. Well now you have a hole in the wall of the intestine. So that also doesn’t really work well. That’s more so why the hollow viscus becomes a problem.
Another reason though…you bring up a good point, is too much air. Well, for the ultrasound waves to move appropriately through tissues, they need a fluid medium. So that’s why we put a water bath over the body, and the ultrasound waves go through a water bath.
So it’s like the same type of thing if one is pregnant, you put gel on the end of the ultrasound tip and goes on the body, or if you have a breast ultrasound, you put gel on the end of it and it goes through the body. You don’t just do it without any sort of fluid or liquid medium there. And that again, because the ultrasound doesn’t move well through that. It’s part of the challenge that we don’t treat through lung because if you have air in the way…because the lung sits on top of the liver. So if you have air in the way it can get in the way, so to say, of the treatment.
Jamie DePolo: I see. And what about bones? They’re not really hollow, but they do have things inside. So, I'm assuming it’s not used to treat any tumors in the bones.
Dr. Brock Hewitt: Great question again. So we do not currently use it to treat lesions in bones, as in the bone being the destination of the ultrasound.
However, the liver, for example, is covered by many ribs and we can treat through a rib to get to the lung tissue behind it. So if the lesion is behind a rib, for example, there are ways…or at least partially blocked by a rib, there are ways we can still treat that lesion.
So it’s a little bit of a difference because the way the ultrasound works and the way the focal point is of the treatment area, is that’s the important part. So if the focal point, for example, is in the bone, that’s different than if the ultrasound has to pass through bone to get to the focal point. It’s kind of like as we start to expand the technology or the implementation of the technology, for example, the pancreas. The pancreas is an organ that sits deep in the body. So the ultrasound waves have to go through many different types of tissue to get to the pancreas, but it can go through multiple different types of tissue without injuring it and that’s kind of a similar thing with the ribs for liver lesions. It can move through the ribs and then get to the target tissue behind in the liver.
Jamie DePolo: Okay. But you wouldn’t use histotripsy right now, say, to treat a cancer lesion in a bone if cancer had metastasized to the bones?
Dr. Brock Hewitt: Correct. Not currently. It will not be used to treat a bone lesion.
Jamie DePolo: Okay. So, how common is it for histotripsy to be used to treat breast cancer lesions in the liver? Does the tumor have to have certain characteristics? Or the person not be a candidate for traditional surgery? How is that decided?
Dr. Brock Hewitt: The FDA indications are thankfully quite broad. So like I mentioned, primary or secondary tumors, of which breast cancer is a secondary tumor to the liver. So as far as, well, what makes a patient a candidate for histotripsy? It doesn’t necessarily matter whether the underlying disease is a breast cancer or a colon cancer. It’s more important about the specific characteristics of those liver lesions. And so, a couple of them is that the size of a single treatment for a liver tumor is around 3.5 to 4 centimeters. Now that being said, if you have a liver lesion that’s larger than that, you can do overlapping treatments during the same session.
Like for example, we’ve treated lesions up to 6 centimeters, and what you do…and other centers have treated even larger to varying degrees. What you do is, is you overlap a treatment. So you treat one area and then you move the device over and treat another area. And then you can treat even a third or fourth area. So what you can do is…the treatment zone is around…it’s about a…it’s spherical or elliptical in shape. You can adjust the treatment size. And so when you make those adjustments, you basically just have to appropriately overlie spheres or ellipses and then you can treat a larger lesion.
And then, as far as anything else additional, it really kind of comes back to, is there value in treating these lesions? Because again, we know that these lesions, especially if they’re breast cancer, but they’ve come from the breast. So we know by definition it is stage IV, it is metastatic disease. And so just because we can do something doesn’t necessarily mean we should do something. And I'm happy to go into more detail about that, but that’s the bigger concern when we’re offering any sort of intervention to any patient: Is the potential benefit of the treatment greater than the risk of the treatment? The nice thing about histotripsy is the risks, comparatively are quite low, especially when you talk about comparing it to something like surgery.
Jamie DePolo: Sure. And so, what would that be? I mean, would you look at, is the tumor causing symptoms? Is it affecting quality of life? Because as you just said, it sounds like the side effects, or the potential risks of histotripsy, seem, just to my unknowledgeable ears, seem slightly low. So I'm wondering why wouldn’t you do it if somebody did have liver lesions?
Dr. Brock Hewitt: Yup. So, the risks are low. They’re not zero, but they are low and I’ll talk about that in a little bit. But to more directly address your question, is why wouldn’t you do it? So there’s two main reasons why you're going to treat something in the liver. Okay? Or at least in this case that you brought up. You hit the nail on the head with one of them. So when we’re talking about offering therapy to anybody in medicine, we really focus on two things. Can we improve the quantity of someone’s life, or can we improve the quality of their life?
So, you mentioned causing symptoms, causing problems. That is called palliative. Now I know that word kind of has a negative connotation sometimes. All it simply means is directly addressing the symptoms or directly addressing that underlying issue, right? So, to your point, if you have a liver…a breast cancer lesion in the liver that is compressing the bile ducts that is causing the bilirubin, for example, to go high and you're unable to get chemotherapy or any other type of therapy, you can treat that one specific lesion, shrink it down, and improve the blockage or remove the blockage in a way, such that now your bilirubin goes down and now you can get therapy again. Right?
Or if a lesion is on the surface of the liver, sometimes those lesions can cause pain and discomfort, and so you can treat that lesion to shrink it down. So the intent of treating those lesions isn’t to cure the patient, but it is to relieve their symptoms, whether the symptom is physical discomfort or whether the symptom is an abnormal lab value. So that is what we call a palliative indication and that is a very reasonable thing to do, okay, with this.
The next question that comes up, and this is the one that’s more hotly debated, is, particularly for people with breast cancer, can we improve the quantity of someone’s life. Okay? And that there’s a lot of debate on. And so, you know when it comes to improving for palliative indications, we just have to keep in mind that the side effects of histotripsy are roughly around 5% in terms of major issues. And so what are some of those major issues? It would be developing something like an abscess or an infected cavity. It would be risks related to bleeding and risks related to the opposite of bleeding, blood clots.
Now again, they're all quite low and comparative if not better than other ablation technologies. And as a surgeon, I can, you know, say this. It’s certainly less risky than a surgery, you know, to remove those lesions. But at the same time, it’s not zero. So you know, 3% to 5% is a very real number to the people that experience it. And you know, if you get something like an infection, you know, that means you have to stay off of your therapy. And we know, again, since this is a metastatic disease we’re talking about for breast cancer, that is potentially life shortening. And so again, if it were zero, I would absolutely agree, let’s see what we can do. But we do need to be deliberate in terms of doing these things because there are, even though low, there are complications in some patients.
Jamie DePolo: Okay. Thank you for that. It sounds like you just target one tumor at a time or is it possible…I think this is called CT fusion, where you overlay a CT scan and target more than one. Is that something that happens?
Dr. Brock Hewitt: Yeah. So, two different points there.
So yes, you can…you only treat one lesion at a time or if the two lesions are close enough and small enough, you can treat them together within one treatment zone, we’ll say. But one treatment period, you can treat multiple tumors. So for example, the most we’ve treated at one time was six lesions. So you treat a lesion, and then you reposition the device, you treat another lesion, and reposition the device, so on and so forth. Usually when we get to around five lesions or so we consider doing it in two different sessions. So we would treat somebody that same day, treat up to five lesions, and then treat multiple lesions again in the future if it’s reasonable or if the person is getting a good response from that.
And so in theory, there’s not really a limitation to how much we can treat because unlike thermal ablations, which essentially act like a nuclear bomb and destroy everything within a certain radius, histotripsy is very precise. It destroys the tissue that is being targeted and then what happens is, over time, the normal liver tissue is preserved a little bit better and it kind of…the term we use for that is hypertrophy, but it essentially grows whereas the tumor itself shrinks. So in theory you get preservation of more normal liver and shrinkage of the tumor. And so you know, in theory, as long as you have a healthy, functioning liver you can over time treat or offer many sessions, in theory.
And then the second point that you brought up about CT fusion. So CT fusion is an option with the device. That is more so directed for if you are having a difficult time seeing it…seeing a tumor on ultrasound, you can use CT fusion because CT and MRI are better modalities than ultrasound at visualizing liver tumors. For example, we may see say an 8-millimeter lesion quite clearly on CT scan, but when we go to ultrasound, we can't quite see it. And if we can't see it, it becomes very difficult to treat. And so, CT fusion is a way to overlay the CT scan on the patient and then you can at least get in a close ballpark and try to target the lesion that way.
Jamie DePolo: Okay. Thank you. I'm curious, when you talk about a treatment session, is there an average time for that? How long does that take?
Dr. Brock Hewitt: Yeah. As the technology has gotten better, the average time has decreased. So what happens is, the way to think of a treatment is that I mentioned a focal area of treatment. So you know, it has increased or the volume of a single area has increased over time. So for example, initially the bubble cloud, which is the treatment focus, that was 3 millimeters x 3 millimeters x 6 millimeters. So kind of like a cylinder. And what happens is, it treats that area, then it moves over a millimeter, and then it treats that area, and then it moves over a millimeter, and so on and so forth. So it does all these little micro treatments over time and it’s that…the movement is done by the computer. It’s kind of like a set it and forget it.
Once you target it and hit the start button, the technology advances on its own. Now you can make real time changes to that. As in if you’re watching it and you don’t feel an area was adequately treated or the patient coughed or whatever it may be, you can make a real time adjustment. So you don’t have to wait until after the procedure is done to then go back and treat again. You can make that adjustment in real time. And so as the technology has gotten better, those treatment zones have gotten a little bit bigger, which means the treatment can move faster. So for example, when we were first starting, like at NYU when we did our first patient in February 2024, our average treatment times were about an hour and some of them it took 90 minutes, which means the patient had to stay still for that long.
Now the patient is asleep. It is general anesthesia currently, and that’s because we want to paralyze the diaphragm. The diaphragm is the muscle that lays on top of the liver. So if that’s moving a lot, that means the liver is moving a lot and that means it’s very difficult to hit a moving target. So we have to paralyze the diaphragm and breathe for the patient and then we can treat the liver, it’s a little more still. And so over time, the treatment periods have gotten much, much shorter and now our average treatment time is 20 minutes or less.
Jamie DePolo: Oh, wow. Okay. Well, that’s great. How successful is histotripsy in treating…and I'm going to ask specifically about breast cancer metastases, but if it has to be more general that’s fine. In treating these lesions in the liver, do we know or is there any research on how long a tumor stays suppressed or, with histotripsy? Do we know that?
Dr. Brock Hewitt: Yeah. Absolutely. So, when you're talking about how effective something is that gets to the point that we had briefly talked about earlier about improving quantity. So when we talk about improving quantity of life, we talk about how effective a therapy is, and there’s two parts to that question. So how effective something is determines, one, how good is it at doing what it’s intended to do? And that means destroying the tumors. And then, the second part of that is, does destroying that tumor effectively, so completely, does it improve the quantity of life, right?
So the first part is really kind of what you're asking, how effective is this treatment? And what we’ve done is — although the treatment has only been around for a little over two years now in terms of active practice — so, we don’t have obviously information longer than that, but we do have pretty good one-year data, which means we’ve looked at a number of centers. NYU has partnered with a number of other centers across the country, and we have published on this. And so, what we see is after a year of treatment about 90 to 95% or so of the tumors are still dead, which is in line with other treatment modalities. So, other ablation modalities. So, microwave ablation, radiofrequency ablation. Those are…we call that the one-year efficacy rate and that’s just over 90%. So, that’s in line with those other treatment modalities. Okay?
And then, like I said, then the question becomes, well does treating that tumor move the needle in terms of extending life? And that’s a little more hotly debated and difficult to tell for now because, again, it’s only been around for a little over two years. So we don’t know if anybody’s lived three years after treatment because nobody’s had it that long. So yeah, just a little bit over 90% in terms of how effective it is. And that’s with breast cancer as well as other therapies. And right now there’s been over 3,000 to 4,000 treatments worldwide and about 5% have been for breast cancer lesions in the liver. So, we have a decent number.
Jamie DePolo: Okay. Okay. Yeah, and I'm assuming to look at overall survival you’d need five, 10, 15 years of follow up. And I'm assuming that research is ongoing?
Dr. Brock Hewitt: Well in a way, yes. So, there’s an active ongoing registry for patients that they can sign up for if they want to. It’s called the BOOMBOX trial.
Jamie DePolo: I love the name of some of these trials.
Dr. Brock Hewitt: They’re great. It helps you remember them.
And so, the goal of that trial, it’s a post-market surveillance study and what we do is…it doesn’t change whether or not someone gets histotripsy, what it does is it allows us to collect patients’ data. Their imaging data, their outcome data, exactly like you're talking about. And what we can do is, we can look back and the goal is to get 5,000 patients into that study and to say, okay, are the early results consistent with now the longer-term results, right? As in, does it still stay effective after five years? Is that number still around 90% or did it drop to 80%? Were there new complications that arose that we didn’t see before? Things like that.
There are a number of smaller randomized trials that are about to be going on with histotripsy, but really where histotripsy is at in terms of its scientific investigation is really more validation in terms of making sure it’s safe and making sure it is locally effective. And then, once we prove that those are true for more patients, then we have equipoise to say, yes, we can now compare it to other good modalities. Because whenever we’re comparing a new technology to an established technology, we never want to offer an inferior technology, okay, in terms of treatment.
Because, for example, you know, surgery is a great local therapy. You remove something and it’s gone. We know that, right? And so is microwave ablation. If you burn something it stays gone over 90% of the time. And so these are proven modalities. And so if we’re ever going to offer somebody an alternative, we have to at least have a decent amount of evidence that suggests that it is at minimum, equivalent. Because again, we never want to offer somebody something that is inferior.
Jamie DePolo: Sure. You talked a little bit about side effects earlier, infection, are there any other side effects that we should know about with histotripsy?
Dr. Brock Hewitt: Yeah. Those were the biggest ones in terms of infections, in terms of small bleeding risks or something called fistulas, which are connections between the blood vessels. Those are quite rare, but it has happened a time or two, less than 1% of total cases, but again not zero. The blood clot situation that arises are local blood clots. So blood clots within some of the blood vessels in the liver, and those almost always resolve on their own, at least in our experience they’ve resolved on their own. So we don’t have to actively put people on blood thinning medicine for that. We may give them a dose of blood thinning medicine at the time of the procedure. That we do, for example, in surgery. So you know, that’s just to kind of make sure because cancer itself causes the body to throw blood clots. That’s one of the things that it does. It’s called…it creates a hypercoagulable state. That means it increases our risk for blood clots. And so, we have to combat that as well.
Another side effect that has happened for some patients is that when multiple lesions are treated, the destruction of the cells can get into the blood system and then it can clog up the kidneys a little bit and it can cause slight change in the kidney function, but all that is also self-resolving with a little bit of extra fluid. So again, it’s not a permanent damage situation. So these are…all the other complications are more short term or more temporary that usually resolve on their own. For example, in our experience at NYU here, we’ve treated over 80 patients, we’ve treated over 160 lesions, and we’ve only had one patient stay in the hospital longer than 24 hours. The vast majority of our patients leave the same day after the procedure.
The most common side effects from this procedure would be abdominal discomfort that might last a couple days and then some flu-like symptoms, because flu-like symptoms are the inflammation reaction from the treatment that patients may experience. And so, and that is also self-limiting. As in both the slight abdominal discomfort, which is almost always treated with over-the-counter medications, so you know, acetaminophen or ibuprofen, something like that. And then, the flu-like symptoms that can occur. And so, those again resolve within just a couple days.
Jamie DePolo: Okay. That’s all very good to know. My next question is a two-parter, and it came from one of our community members, and I believe this person has liver metastases. So, first part is, could you explain the abscopal effect, and then after we know about that, is there any evidence that histotripsy provides an abscopal effect, which could make immunotherapy more effective on liver mets?
Dr. Brock Hewitt: Yes. That is arguably one of the most hotly debated topics within the histotripsy community. So, excellent question. You certainly have very, very well-informed listeners and community members.
So, what this individual is talking about…what the abscopal effect is, is what we would call an off-target effect. So what I mean by that is, say for example, somebody has five lesions in their liver, say five breast cancer tumors in their liver and you only treat two of them. An abscopal effect, or an off-target effect, would be that all five of them shrink even though only two of them were treated.
And the way that we believe that that happens…I'm saying more broadly, not specifically for histotripsy, but more broadly, if an abscopal effect or if an off-target effect happens, the way we think it happens is that essentially by destroying that tumor our immune system is able to go in and pick up the wreckage and now more appropriately recognize what the cancer actually looks at or what the cancer actually looks like. And then can go to other areas of the body, whether it’s in the liver or even other organs where maybe the tumor might be, and now it recognizes it better. And now it can go and kill it better.
Because our body is the best defense over the vast majority…if we can appropriately educate our body on how to kill things that would be the best-case scenario. That’s why you’ve seen this explosion in immunotherapy over the last decade and a half. Is that’s kind of the holy grail, is teaching our body how to better treat things. Now I am not saying that chemotherapy doesn’t have a role or targeted therapies don’t have a role, they certainly do and they’re currently the backbone of any treatment or any metastatic disease treatment paradigm, but the goal would be to educate our bodies better. So that’s specifically what the abscopal or the off-target effect is, is that tumor that is not actively treated is being better recognized and then destroyed by our own body. And so, does this happen with histotripsy. That’s the question, does this happen with histotripsy?
Jamie DePolo: Right.
Dr. Brock Hewitt: The true answer is, we don’t know. We’re actually right now in a conversation with a number of other centers and we’ve created kind of a research initiative to collect examples of this. However, this is all what we call retrospective, which means we’re looking backwards in time to try to understand this, and anybody who does research understands that when you look backwards in time, you can't account for a lot of factors that may be actually influencing the outcomes. And so it’s difficult to make a direct comparison and say, yes, this abscopal effect is happening.
What we’re doing is we’re collecting information on patients that are on no other therapies and they had some other lesions treated, and all of their disease or other non-therapy sites are improved. Because then we can say, okay, you know, maybe there is some truth to this. At NYU we’re going to be opening up, hopefully later on this year, so it’s not actively open now, but we want to open up a trial. Now, this is in liver cancers, but we want to open up a trial where we are treating liver tumors and then testing the blood for the body’s response to see if we can investigate this on a more concrete level.
To say, yes, if we can show or if we detect increased activity in our own immune system after treating a tumor with histotripsy, then we have some evidence to suggest that maybe there is an abscopal effect or an off-target effect that is happening. But for right now, I would say, we don’t know, but it is a hotly investigated area.
Jamie DePolo: Okay. And then, finally, what about insurance coverage for histotripsy? It sounds like since it is relatively new, it sounds like it’s not available everywhere yet. Is it covered by most or how does that work?
Dr. Brock Hewitt: So in terms of where is it offered. It is being offered at a growing rate at many, many centers, at least 50 that I know of in the United States and arguably more on the way. So as far as coverage goes, it is approved by CMS, so Medicare, Medicaid will pay for this if that’s the insurance you have. Private insurers, it’s a little bit more challenging, but not impossible. I'd say our private insurance coverage rate is around 75 to 80%. So usually what happens is, is we’ll submit for coverage for this. We’ll get a prior authorization. It only comes through about half the time. Then we go the back and forth of doing the appeals process, so on and so forth, and you know half of those get approved. So like I said, it ends up being around — at least in our experience — about 75 to 80%. However, that may vary dramatically by state and the particular payer type. So most patients can get this covered as part of their kind of their treatment plan with insurance.
You know, I have talked with some individuals in the company, and I know this talk has been focused on breast cancer that has spread to the liver. However, the hope is in later 2027-ish, although the timeline is not always concrete, the company that creates this technology are going to be looking at breast primary lesions. So lesions that are in the breasts themselves. They have developed a treatment head. So that’s the device that has the ultrasound probes in them that can treat lesions that are very close to the skin’s surface.
Because right now, the technology…the tumor needs to be at least 2.5 to 3 centimeters deep for it to be treated and that’s a problem with, obviously, with the primary breast cancer because most lesions are around that deep on the vast majority of patients. And so, the technology is advancing. There are a couple steps that need to still be taken before. However, I just want to get that out there to provide hope for patients because the longer you can, again, keep fighting this disease, you know, there’s new technology and new devices right around the corner. So the hope is in a year or two down the line they’ll be able to treat primary breast disease with this technology.
Jamie DePolo: And when you say that, would that be say an early-stage tumor or would it have to be a primary tumor in the breast that has already spread?
Dr. Brock Hewitt: So, that goes back to what I mentioned earlier when we were talking about if we’re going to offer this technology as a substitute for surgery, which is the standard of care in the vast majority of those patients, we’ve got to know it works. So, in the next year or two, what I would say is, it would still be very experimental in that sense. The standard of care for the short term, for at least the next couple years, at a minimum, will be surgery.
But as we’ve seen with breast cancer, even very early-stage breast cancers, you know, particularly those that are ER/PR-positive, so on and so forth, maybe surgery isn’t needed right away. Maybe you can go with just the hormonal therapy itself and try to control the disease, right? And so…so there are certainly potential options for patients. But I will say currently or any time in the short future, the standard of care will still be surgery. So let me be very clear about that. I just wanted to let people know that this technology is going to be coming out and being tested in that way.
Jamie DePolo: Okay. All right. Thank you so much. This is very exciting. I will definitely stay tuned for that as well.
Dr. Hewitt, thank you so much. This has been so educational, so interesting. I really appreciate your time. And I am going to look forward to some of these studies coming out into publications so we can learn a little bit more. Thank you.
Dr. Brock Hewitt: Wonderful. My pleasure. Thank you so much again for having me.
Thank you for listening to The Breastcancer.org Podcast. Please subscribe on Apple Podcasts, Google Podcasts on Android, Spotify, or wherever you listen to podcasts. To share your thoughts about this or any episode, email us at podcast@breastcancer.org or leave feedback on the podcast episode landing page on our website. And remember, you can find out a lot more information about breast cancer at Breastcancer.org and you can connect with thousands of people affected by breast cancer by joining our online community.
Your donation goes directly to what you read, hear, and see on Breastcancer.org.