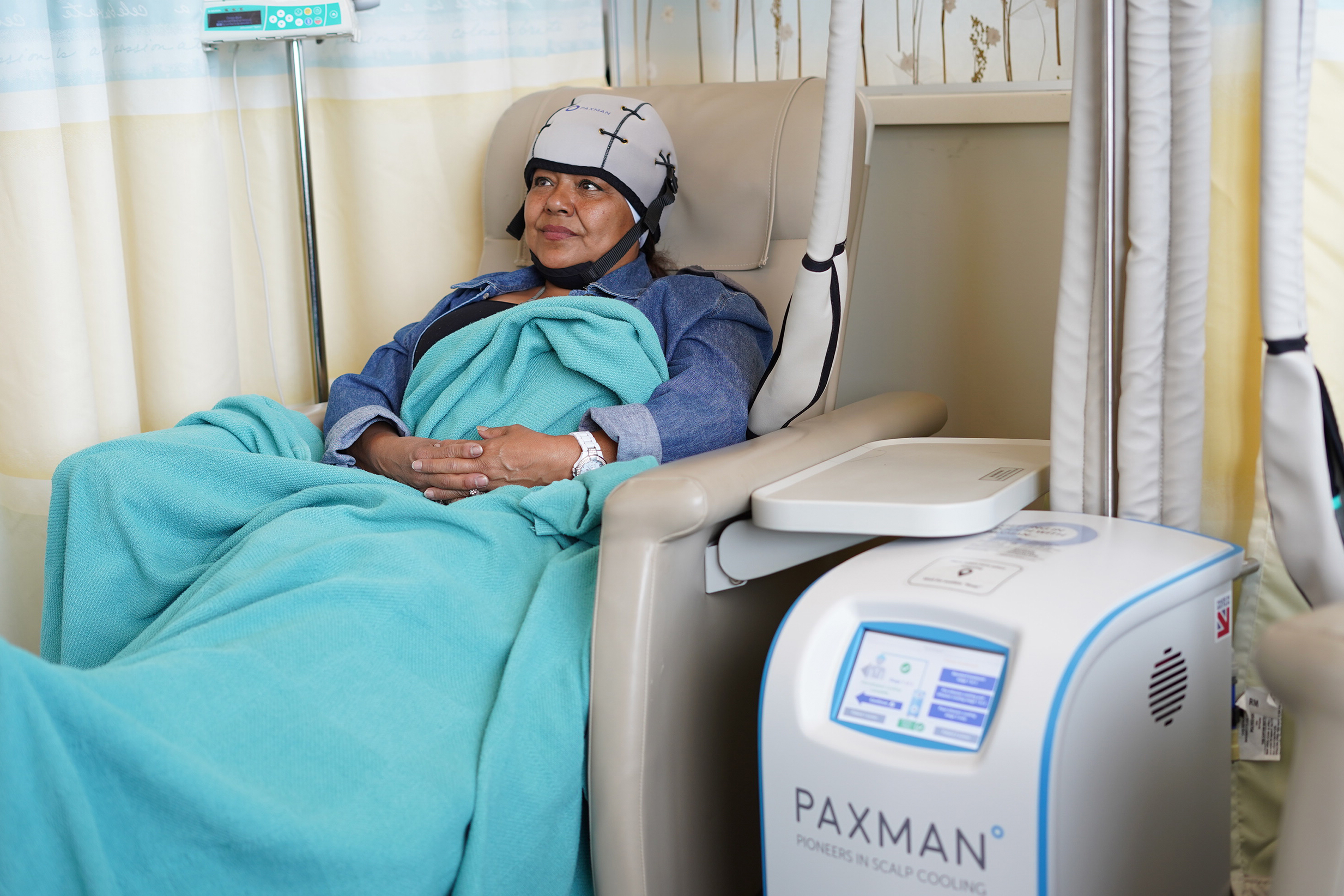
Cold Caps and Scalp Cooling Systems
Cold caps and scalp cooling systems are tightly fitting, helmet-like hats filled with a cold gel or liquid that you wear during chemotherapy infusions. These devices have helped many people keep some or quite a bit of their hair during chemotherapy, which can cause hair loss.
Cold caps and scalp cooling systems work by narrowing the blood vessels beneath the skin of the scalp, which reduces the amount of chemotherapy medicine that reaches the hair follicles. With less chemotherapy medicine in the follicles, the hair may be less likely to fall out. The cold also decreases the hair follicles’ metabolic activity, which makes the cells divide more slowly and protects the follicles from the chemotherapy.
During each chemotherapy session, you wear the cap for 30 to 50 minutes before the infusion, during the infusion, and for a certain amount of time after the infusion. The amount of time you wear the cap after the chemotherapy infusion can vary from 20 minutes to 4 or 5 hours, depending on the type of chemotherapy you’re getting and the type of scalp cooling method you use.
Scalp cooling methods: cold caps vs. scalp cooling systems
There are two main scalp cooling methods: cold caps and scalp cooling systems.
Cold caps
Also called manual cooling systems, cold caps are similar to ice packs. You need to keep cold caps in a cooler with dry ice or in a special biomedical freezer before wearing them. Each cap warms up and thaws while you wear it, so you need to replace it with a new cold cap every 20 to 30 minutes during a chemotherapy infusion session.
Usually, the person who is getting chemotherapy rents the cold caps and brings them to each infusion session in a portable cooler with dry ice. If you’re interested in doing this, you should coordinate with your doctor and cancer treatment facility in advance. You will need a friend, family member, or hired trained “capper” to change the caps for you during each infusion session. If your cancer treatment facility has a biomedical freezer, you may be able to store your caps in the biomedical freezer the night before your infusion session.
There are a few manufacturers that make cold caps, including Penguin Cold Caps, Chemo Cold Caps, and Arctic Cold Caps. Some of these manufacturers have posted instructional videos on their websites or YouTube channels that can help you and the person who is assisting you understand how to use cold caps.
Scalp cooling systems
Also called automated cooling systems, scalp cooling systems use a cap that is attached to a small, computer-controlled refrigeration machine. The refrigeration machine circulates cool liquid in the cap during the entire chemotherapy infusion session, so the cap doesn’t need to be changed like manual cold caps do.
The three scalp cooling systems currently sold in the United States are the DigniCap System, the Paxman System, and the Amma Portable Scalp Cooling System by Cooler Heads. These machines are located at some, but not all, cancer treatment facilities in the United States, and the cost may vary by location and other factors.
Ask your care team if scalp cooling systems are available at the facility where you’re planning to receive chemotherapy treatment. The Rapunzel Project, a nonprofit organization that helps people access scalp cooling, has a list of cancer treatment centers in the United States that have scalp cooling systems or biomedical freezers for cold caps.
The Paxman System and the Amma Portable Scalp Cooling System require you to provide them with a prescription for scalp cooling from your doctor before you can sign up.
Some people have successfully gotten their health insurance to cover some of the cost of renting cold caps or scalp cooling systems. But insurance coverage for scalp cooling isn’t yet standard in the United States.
Preparing for scalp cooling
Whether you use cold caps or a scalp cooling system, it’s important to make sure the cap fits correctly to increase the chance it will be effective. Carefully follow the manufacturer’s instructions on how to fit the cap on your head, and practice before your first treatment. If you have curly or kinky hair and notice the instructions don't seem to apply to your hair type, be sure to discuss how to get the best fit with your healthcare team.
Both scalp cooling methods get very cold, so some people get headaches while wearing the caps. Other possible side effects include:
neck and shoulder discomfort
scalp pain
forehead pain
dizziness
nausea
Most people get very cold during scalp cooling, so you should dress warmly and bring warm blankets with you, or ask the cancer treatment center if they have blankets you can use. People tend to feel colder wearing cold caps than they do using scalp cooling systems. It’s common for people to feel the most discomfort during the first 10 minutes of treatment and then feel less discomfort as they adjust to the cold.
When using cold caps or a scalp cooling system throughout chemotherapy treatment, it’s smart to be extra gentle with your hair to prevent damage and help maintain hair quality. It’s recommended that you:
use a gentle shampoo
comb and brush gently
avoid dyeing your hair until three months after chemotherapy is done
avoid using blow dryers, hot rollers, and straightening irons
Research on scalp cooling
Some doctors have expressed concern that scalp cooling methods could prevent chemotherapy medicine from reaching cancer cells that may have spread (metastasized) to the scalp. But it’s rare for breast cancer to spread to the scalp. And multiple studies that compared patients who used scalp cooling techniques with those who did not found no difference in the number of scalp metastases between the groups. 1 2 3 4
The U.S. Food and Drug Administration (FDA) has cleared the DigniCap Scalp Cooling System, the Paxman System, and the Amma Portable Scalp Cooling System by Cooler Heads, which means these scalp cooling systems can be sold in the United States.
The effectiveness of scalp cooling varies, depending on a number of factors, including the type of chemotherapy you receive and the dose. Some chemotherapy medicines commonly used to treat breast cancer include:
anthracyclines, such as Adriamycin (chemical name: doxorubicin) and Ellence (chemical name: epirubicin)
taxanes, such as Taxol (chemical name: paclitaxel), Taxotere (chemical name: docetaxel), and Abraxane (chemical name: albumin-bound or nab-paclitaxel)
Women who received taxane chemotherapy alone without an anthracycline chemotherapy medicine have had better results with cold caps and scalp cooling systems than women who received anthracycline chemotherapy.
According to a study that led to FDA clearance for the Paxman scalp cooling system in 2017, about 59% of the women who received scalp cooling while receiving taxane-based chemotherapy lost less than half their hair and about 16% of the women who received scalp cooling while receiving anthracycline chemotherapy lost less than half their hair. 5 According to research that led to the FDA clearance of the DigniCap System in 2015, about 66% of the women who received scalp cooling while receiving taxane chemotherapy lost less than half their hair. 6 The study didn’t look at women who were receiving anthracycline-based chemotherapy.
If you’re interested in trying cold caps or a scalp cooling system, talk to your doctor about all the factors that you need to take into account, including your chemotherapy regimen, possible side effects, costs of scalp cooling methods, and any other health issues you might have. You may also want to consider that some people feel using cold caps or a scalp cooling system gives them a sense of control during cancer treatment, regardless of how much hair they retain. A study in Ireland found that the majority of people who tried scalp cooling during chemotherapy were satisfied with their choice to do so, whether or not it was effective for them. 7
![[object Object]](/_next/static/media/art.00u0jy8p9yebo.png?dpl=dpl_8WWA71LCFM991WJJwscsH7guGagH)
Using Cold Caps During Breast Cancer Treatment
Dec 18, 2020Covering the cost of scalp cooling
The cost of using cold caps or scalp cooling system varies depending on the manufacturer, the number of chemotherapy sessions you have, and the number of months you need to use the scalp cooling method.
Cold caps typically cost about $380 to $450 per month, plus shipping costs and a refundable security deposit in some cases. Scalp cooling systems can cost from $2,000 to $2,200 for a full course of chemotherapy. Some cancer centers also charge a facility fee each time you use their scalp cooling system during a chemotherapy infusion.
Insurance coverage for scalp cooling is not yet standard in the United States, but some people have successfully gotten their health insurance to cover some or all of the cost. Aetna is one health insurance company that considers scalp cooling to prevent hair loss during chemotherapy to be a medically necessary, covered expense (although whether it’s covered depends on your individual health plan). Check with your health insurance company to find out their policies. Also, contact the manufacturer that makes the cold cap or scalp cooling system you plan to use for advice on how to submit a claim to your health insurance company for reimbursement. Learn more about insurance coverage for the DigniCap system and about insurance coverage for the Paxman system.
If you need help paying for a cold cap or scalp cooling system, find out if the medical center or clinic where you’ll be receiving chemotherapy offers financial support for people using scalp cooling methods. Also, the Hair to Stay Foundation and Sharsheret offer need-based grants to pay for some scalp cooling costs.
The Rapunzel Project is a nonprofit organization that helps people who are getting chemotherapy access and use scalp cooling technology to help keep their hair. Visit The Rapunzel Project for more information.
The Breastcancer.org community has tips and advice for managing chemotherapy side effects, so consider joining the conversation.

Ross M, Fischer-Cartlidge E. Scalp Cooling: A Literature Review of Efficacy, Safety, and Tolerability for Chemotherapy-Induced Alopecia. Clin J Oncol Nurs; 2017. Available at: https://doi.org/10.1188/17.CJON.226-233
Rugo HS, et al. Scalp cooling with adjuvant/neoadjuvant chemotherapy for breast cancer and the risk of scalp metastases: systematic review and meta-analysis. Breast Cancer Res Treat; 2017. Available at: https://doi.org/10.1007/s10549-017-4185-9
Rugo HS, Voigt J. Scalp Hypothermia for Preventing Alopecia During Chemotherapy. A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Clin Breast Cancer; 2017. Available at: https://doi.org/10.1016/j.clbc.2017.07.012
Kruse M, Abraham J. Management of Chemotherapy-Induced Alopecia With Scalp Cooling. J Oncol Pract; 2018. Available at: https://doi.org/10.1200/JOP.17.00038
Nangia J, et al. Effect of a Scalp Cooling Device on Alopecia in Women Undergoing Chemotherapy for Breast Cancer: The SCALP Randomized Clinical Trial. JAMA; 2017. Available at: https://doi.org/10.1001/jama.2016.20939
Rugo HS, et al. Association Between Use of a Scalp Cooling Device and Alopecia After Chemotherapy for Breast Cancer. JAMA; 2017. Available at: https://doi.org/10.1001/jama.2016.21038
Maher W, et al. The uptake, patient satisfaction and efficacy of scalp cooling among patients receiving chemotherapy in an Irish oncology day ward. Poster presented at: ESMO 2019 Congress; Sept. 28, 2019; Barcelona, Spain. Available at: https://oncologypro.esmo.org/meeting-resources/esmo-2019-congress/The-uptake-patient-satisfaction-and-efficacy-of-scalp-cooling-among-patients-receiving-chemotherapy-in-an-Irish-oncology-day-ward