DIEP Flap Reconstruction Procedure
What is DIEP flap surgery?
DIEP flap surgery is a breast reconstruction procedure that uses a flap of tissue that’s removed from the lower belly and transferred to the chest to rebuild one or both breasts.
The tissue flap that the surgeon transfers includes skin, fat, blood vessels, and sometimes nerves. Using microsurgery, the surgeon connects the blood vessels in the flap to the blood vessels in the chest, creating a reconstructed breast with its own blood supply.
The DIEP — or deep inferior epigastric perforator — flap is named for the blood vessels that run from the abdominal muscle through the fat, and into the skin.
DIEP flap surgery is the most popular, commonly done flap reconstruction procedure.
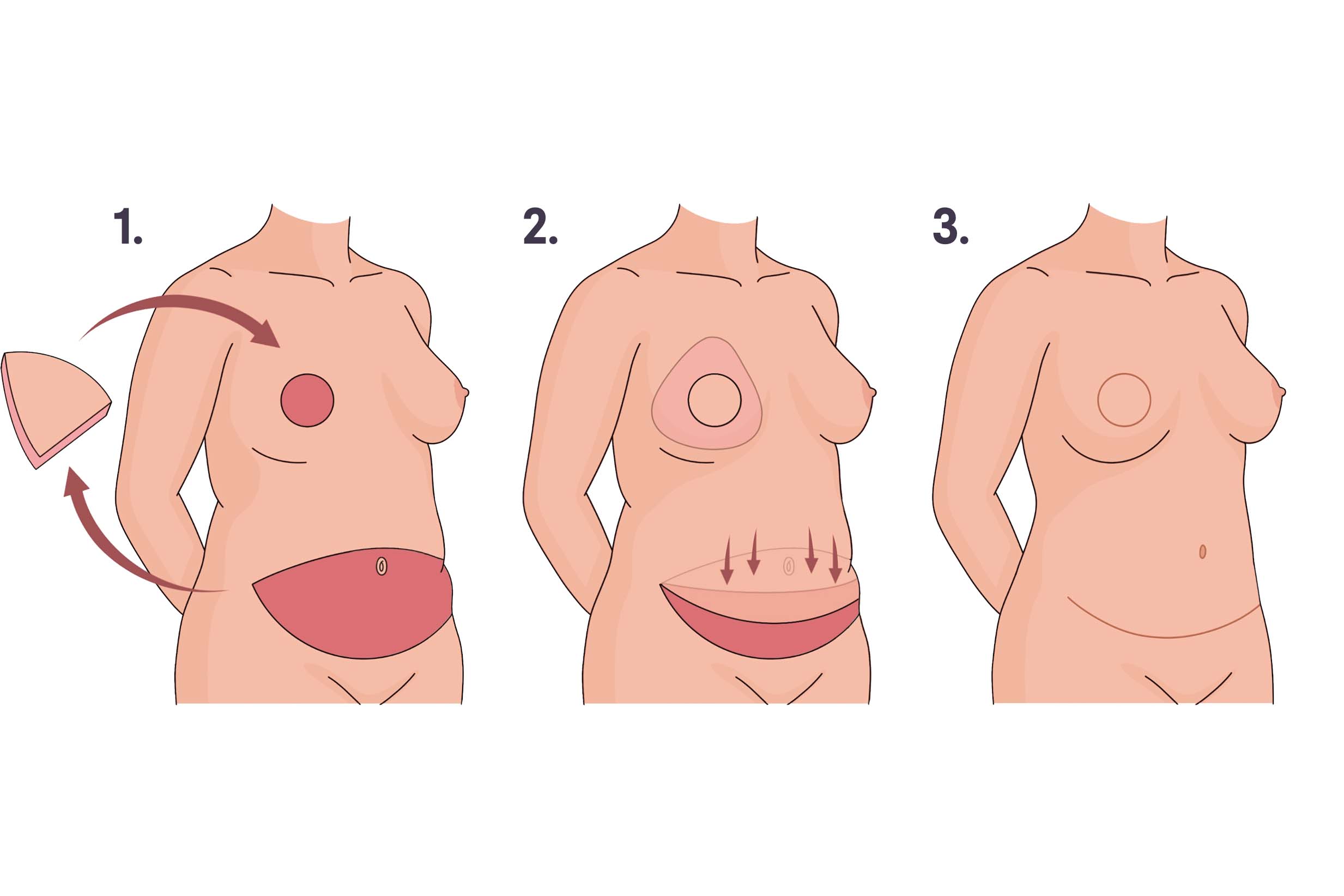
1. Breast tissue and nipple are removed and a flap of tissue is removed from the abdomen. 2. The flap is moved to the chest to create a breast mound, and blood vessels in the flap are connected to blood vessels in the chest. The abdominal skin is pulled down and the belly button is repositioned. 3. Incisions in the breast and abdomen are closed. Illustration by You Jeong (Julie) Park, MD.
What are the benefits of DIEP flap surgery?
As with other flap reconstruction techniques, DIEP flap surgery offers several advantages over reconstruction with implants. For example, a reconstructed breast made from your own tissue might look and feel more natural and softer than one reconstructed with an implant. And while implants may need to be replaced one or more times, flap reconstruction generally lasts a lifetime.
Also, some people like that after a DIEP flap surgery, your belly looks flatter and feels tighter — as if you’d had a tummy tuck.
Research suggests that many people who get DIEP flap surgery report a high rate of satisfaction.
DIEP flap reconstruction is usually a better choice for most people than a similar procedure called TRAM flap reconstruction. TRAM flap surgery involves removing muscle, so it has a higher risk of complications (such as abdominal wall weakness or hernia) and recovery takes longer.
What are the downsides of DIEP flap surgery?
The main disadvantage of DIEP flap reconstruction, compared with implant reconstruction, is that it’s a much longer and more complex surgery with a longer recovery time. There are more incisions to heal because there are two surgical sites.
There’s also a higher overall risk of complications with DIEP flap surgery than implant reconstruction.
Is DIEP flap surgery right for you?
DIEP flap surgery may be a good option for you if:
you have enough fat in your lower abdominal area to build a breast that’s the size you want
you want to avoid the potential complications and the maintenance requirements of implants (such as periodically checking for rupture with ultrasound or MRI if you have silicone implants)
you’re having your breast implants removed and want another type of reconstruction
DIEP flap surgery may not be right for you if:
you’ve already had certain abdominal surgeries, such as ventral hernia repair, laparotomy, liposuction, or tummy tuck (abdominoplasty)
your abdominal blood vessels are small or aren’t in the best location to do a DIEP flap
you have certain health conditions, such as heart or lung problems or a history of pulmonary embolism or deep vein thrombosis, that could make flap surgery unsafe for you
you want to avoid the specific potential complications that are associated with DIEP flap surgery
Options if you’re interested in DIEP flap surgery but don’t have enough extra abdominal fat
If your doctor tells you that you don’t have enough extra abdominal fat for a DIEP flap, ask them about other options such as:
reconstruction with a different kind of flap, such as a PAP flap, LTP flap, or TUG flap
stacked flap reconstruction, which uses two flaps to build each breast (for example, taking tissue from both sides of your belly instead of from the middle or taking tissue from both the belly and from the thighs or buttocks)
hybrid breast reconstruction (which uses a flap of tissue and a small breast implant to rebuild the breast)
fat grafting to add volume after the initial reconstruction surgery
What to expect with DIEP flap surgery
DIEP flap surgery can be done at the same time as a mastectomy (called immediate reconstruction) or as a separate surgery that is done weeks, months, or years later (called delayed reconstruction). Your medical team can help you decide on the timing that works best for your individual situation and treatment plan.
Before DIEP flap surgery
Your surgeon may ask you to get imaging tests — such as a computed tomography angiogram (CTA) or a magnetic resonance angiogram (MRA) — so that they can evaluate the blood vessels in your abdomen. This may be done to check if you’re a good candidate for DIEP flap surgery or to help plan the surgery.
If you’re getting delayed DIEP flap reconstruction, you may be advised to get temporary breast implants called tissue expanders at the time of the mastectomy. Tissue expanders can help preserve or expand the breast skin (including during radiation therapy, if that’s part of your treatment plan). The tissue expanders will be removed during the DIEP flap surgery.
When preparing for your DIEP flap surgery, it’s a good idea to come up with a plan for how much time you’re taking off work or other activities and for getting support from caregivers during your recovery. Also, in the weeks leading up to surgery, doing exercises that strengthen your core, back, arms, and cardiovascular health can help reduce the risk of complications and shorten your recovery time.
Your surgical team will give you instructions on what to do before you have surgery (called pre-op instructions). These may include adjusting the medicine you take, not eating or drinking after a certain time the day before your surgery, and showering with a special antibacterial skin cleanser. If you smoke, you’ll be advised to stop smoking or taking any nicotine products for as long as possible before the surgery. Smoking increases the risk of serious surgical complications, including flap failure.
During DIEP flap surgery
DIEP flap surgery on one or both breasts can take from four to six hours or more. The surgery may take longer if it’s done at the same time as a mastectomy.
You’ll receive general anesthesia through an IV in your hand or arm.
The surgeon will make an incision in the lower abdomen and remove a flap of tissue that includes skin, fat, and blood vessels. Then the surgeon will transfer the tissue to the chest to form one or two new breasts. The surgeon will attach the tiny blood vessels in the flap to the blood vessels in the chest using microsurgery and shape the tissue. Then they will stitch the new breast(s) into place and close the incisions in the chest and abdomen with stitches or staples.
There will be additional steps to the surgery if you’re getting a stacked DIEP flap procedure or hybrid breast reconstruction (which involves adding a flap over a breast implant).
Usually, the surgeon will place surgical drains in the incisions in the chest and abdomen to collect excess fluid. These will be removed two to four weeks later.
It’s possible that during your surgery, your surgeon will find that they can’t complete a DIEP flap procedure due to the position and flow of blood in your blood vessels. (Your surgeon should discuss the possibility with you that they might have to change their plan mid-surgery as part of the informed consent process before the procedure). Instead, they may switch to doing, for example, a SIEA flap, a TRAM flap, or an APEX flap.
The abdominal incision for DIEP flap surgery leaves a scar that runs horizontally from one hip to the other and is located about one-third of the way up between the pubic bone and the navel.
After DIEP flap surgery
After surgery, you’ll be taken to the recovery room, where staff will monitor your heart rate, body temperature, blood pressure, and pain level.
DIEP flap surgery typically requires a hospital stay of two to four days. The surgical team will monitor the flap to make sure it’s getting enough blood supply.
The surgical team will also give you instructions to follow before you leave the hospital (called post-op instructions), including recommendations for how to care for the dressings, sutures, and surgical drains. They will give you prescriptions for pain medicines to take when you get home (usually this will include narcotic and non-narcotic pain medicines).
Recovery from DIEP flap reconstruction
Recovery from DIEP flap surgery can take from 6 to 8 weeks.
To lower the risk of blood clots after surgery, your surgeon may prescribe daily injections of a medicine called Lovenox for 5 to 10 days after the surgery. The injections are given under the skin of the abdomen, buttock, or thigh.
Because you’ve had surgery on two different parts of your body (your chest and your belly), you might feel worse than someone having mastectomy alone and/or reconstruction with implants and it may take longer for you to recover. You will have incisions on your breast(s), your lower abdomen, and around your navel, and you may have drains in your reconstructed breast and in your abdominal donor site. If you had axillary lymph nodes removed, you may have an incision under your arm as well.
Be sure to keep your incisions clean, dry, and protected and follow your surgical team’s instructions on when to start walking, stretching exercises, and regular daily activities.
During the first week after surgery, it’s normal to have difficulty or pain when you move (including when you sit down, stand up from a sitting position, or get in and out of bed). Your doctor can show you how to move until you heal.
It’s also normal to have some numbness and tingling in the area of the incisions in your chest and belly, which can last for months.
You may want to ask your doctor for a referral to a physical therapist, who can help you regain your mobility and strength and manage post-surgical pain.
It can take as long as a year or more for your tissue to completely heal and for your scars to fade.
DIEP flap surgery risks and complications
Possible complications of DIEP flap surgery include:
Tissue flap necrosis: when the flap doesn’t get enough blood supply and part or all of it dies. If most or all of the flap develops necrosis, then the surgeon will need to remove the flap.
Fat necrosis: when some of the fat in the flap doesn’t get enough blood supply and it gets replaced by firm scar tissue that can feel like a lump.
Hernia: when a hole develops in the abdominal wall, allowing part of an organ (such as an intestine) to bulge out. (Also, some people may just develop an area of weakness in the abdominal wall). If you develop a hernia or weakness, it tends to become noticeable about a year or more after the surgery.
Call your doctor right away if the flap turns black or blue or develops open wounds, or if you have bleeding, fluid drainage from the incisions, severe pain, rapid swelling, or a high fever.
Learn more about possible complications after flap surgery.
Follow-up procedures after DIEP flap surgery
Once your reconstructed breasts have healed — about four to six months after your DIEP flap surgery — you might decide to have other procedures to improve the results. For example:
fat grafting, which can be used to fill in imperfections, add volume to the reconstructed breast(s), or improve skin affected by radiation therapy
corrective surgery to make scars from breast surgeries less visible, to correct asymmetry, or to address a complication that might have resulted from DIEP flap surgery
It’s important to know that usually you can only use tissue from the lower belly to rebuild your breast(s) once. Once you’ve had a DIEP flap or another type of abdominal wall flap reconstruction procedure, your surgeon would need to use a flap from another part of your body if you were to ever get flap surgery again.
Finding a surgeon for DIEP flap reconstruction
DIEP flap surgery is done by a board-certified plastic surgeon with specialized experience and training in microsurgery. Not all plastic surgeons who do breast reconstruction offer DIEP flap surgery, and the procedure is not as widely available as implant reconstruction. Ask your cancer care team to refer you to plastic surgeons specializing in DIEP flap reconstruction. You can also search for plastic surgeons who specialize in DIEP flap reconstruction in your area using the American Society of Plastic Surgeons directory.
Paying for DIEP flap reconstruction
In some cases, it might take some persistence to find a surgeon to do DIEP flap surgery who takes your insurance and to get your insurance to fully cover the procedure. Not all insurance companies reimburse plastic surgeons for the procedure at the same rates. If your insurance company has low reimbursement rates for DIEP flap, that can make it more difficult to find a plastic surgeon to do your surgery. Also, some plastic surgeons who perform DIEP flap surgery don’t accept insurance and will only work with patients who can pay out of pocket for the full cost of the procedure. Another issue that can come up is that you might find that the plastic surgeon you want to work with does take insurance but isn’t in your plan’s network.
Keep in mind that there are some state laws and a federal law called the Women’s Health and Cancer Rights Act of 1998 (WHCRA), that require certain types of health insurance plans that pay for mastectomy to also cover breast reconstruction.
Learn more about breast reconstruction insurance and payment issues.
DIEP flap before and after images
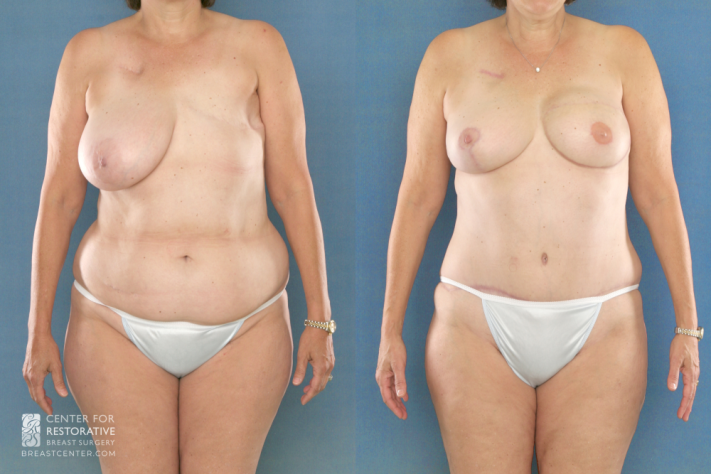
DIEP flap reconstruction on left breast with right breast reduction to C-cup size for symmetry.
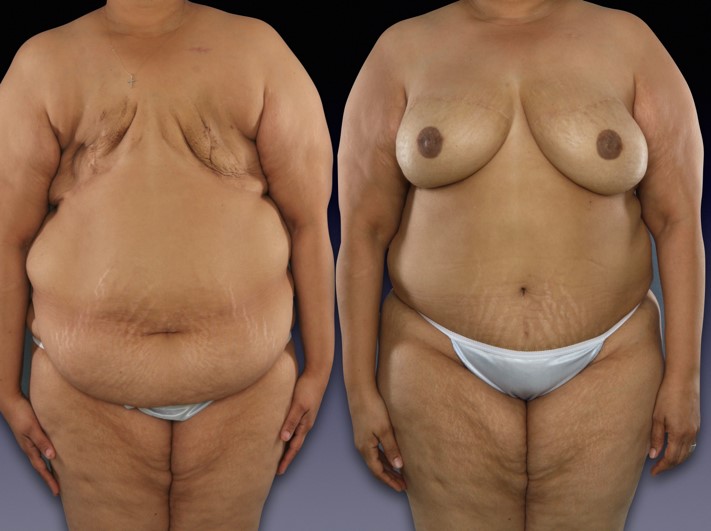
Before and after bilateral delayed DIEP flap reconstruction.

This information made possible in part through the generous support of www.BreastCenter.com.